Follow us on LinkedIn
If you're planning to build a telemedicine app — whether you're a healthcare startup mapping your first product, a hospital system expanding into virtual care, or a digital health company adding remote capabilities — this guide is written for you.
Healthcare systems are under pressure. Physician shortages are projected to reach tens of thousands in the coming years, while millions of people live in areas with limited access to mental health and specialty care. As telehealth becomes part of the response, in this article, you'll find a complete step-by-step overview of how to approach such products strategically and responsibly.

What is a telehealth app?
A telehealth platform lets patients and healthcare providers stay connected from a distance through video calls, phone consultations, secure messages, and digital monitoring tools. At its core, telemedicine app development focuses on enabling safe, compliant, and structured remote care.
Live consultations, asynchronous messaging, digital prescriptions, remote diagnostics, and EHR access are all possible through telemedicine apps — integrated with cloud infrastructure to store and transmit PHI securely under HIPAA and GDPR.

Telemedicine market overview & key trends
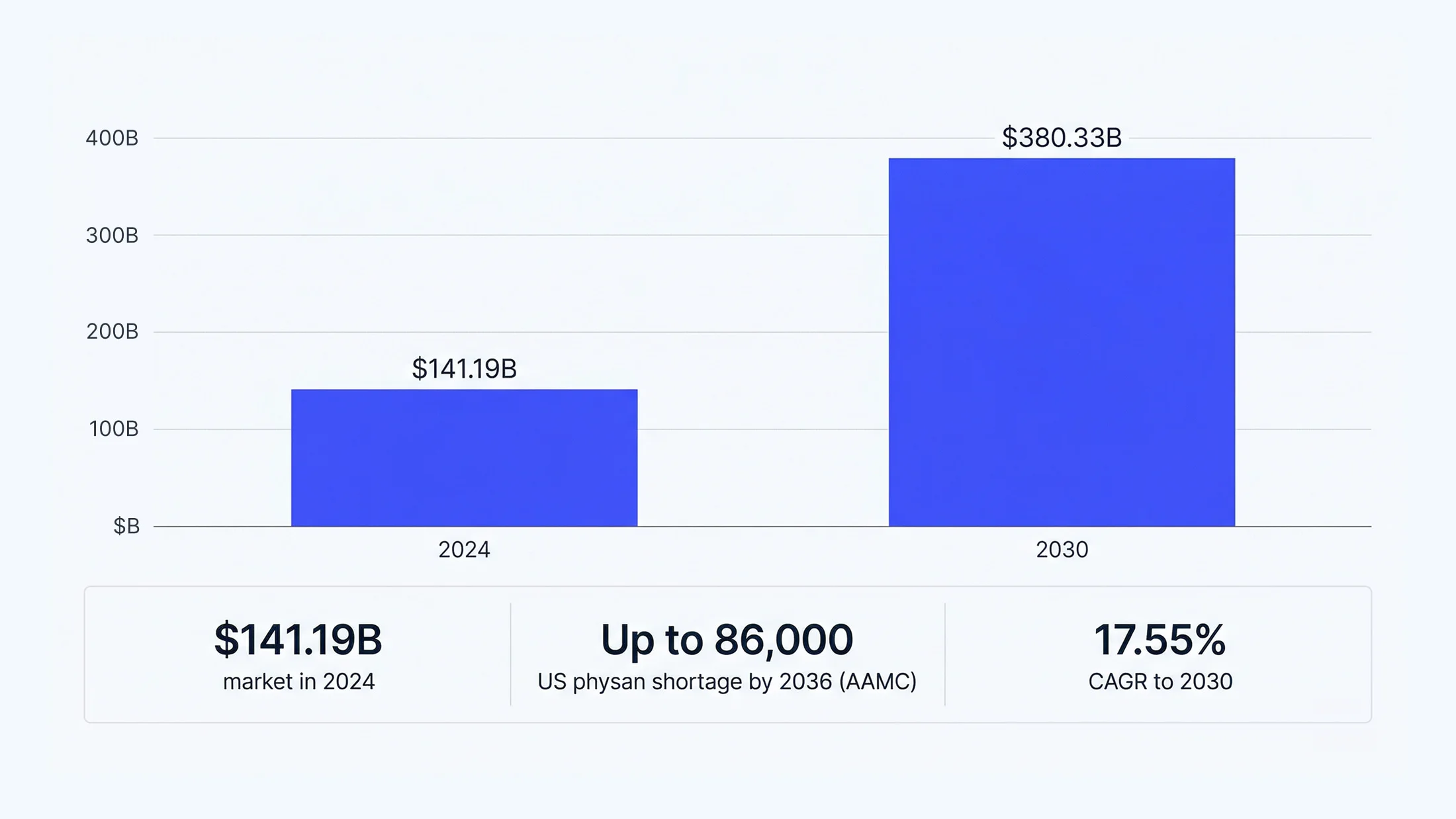
The telehealth market has shifted from pandemic-era spike to sustained structural growth. The global market was estimated at $141.19 billion in 2024, projected to reach $380.33 billion by 2030 (CAGR 17.55%) — driven by physician shortages, aging populations, and the permanent normalization of hybrid care. The AAMC projects a shortage of up to 86,000 physicians by 2036.
The shift is visible across several structural trends shaping how telehealth is adopted and scaled:
- Behavioral health is leading the adoption. A significant share of telehealth visits focuses on mental health, making telepsychiatry one of the most stable segments.
- Hybrid care is the new standard. Telehealth complements in-person care — used for follow-ups, triage, and chronic disease management.
- AI integration is accelerating. Chatbots, automated intake, and predictive analytics are reducing clinician workload.
- Reimbursement policies shape strategy. Behavioral health and certain remote monitoring services are often permanently covered.
- Remote patient monitoring is becoming billable. Monthly reimbursement models for chronic condition monitoring are expanding.
Types of telemedicine applications
Before investing in telemedicine app development, define which category fits your strategy. Our healthcare app development services can help you align your product's direction with clinical goals. But before that, check out different kinds of telehealth apps.
Clinical telemedicine platforms
Support general medical consultations — video calls, secure messaging, appointment scheduling, e-prescriptions, and EHR integration for primary care, urgent care, and follow-up visits.
Mental health and telepsychiatry services
Licensed professionals conduct therapy sessions, medication management, and crisis assessments via video. Audio-only services remain common for reimbursement scenarios. AI-assisted intake assessments reduce session overhead.
Remote patient monitoring solutions
Collect health data from wearables and transmit it to providers in real time — tracking heart rate, glucose, and blood pressure. Designed around billing codes and compliance requirements for chronic condition management.
Specialty and diagnostic telemedicine
Dermatology, cardiology, oncology, and neurology — each requiring imaging integrations, device compatibility, and domain-specific data processing. Deeper technical integration and specialized clinical knowledge required.
Telemedicine for enterprises and hospital networks
Multi-role dashboards, audit logging, compliance tracking, SSO, and legacy EHR interoperability. Scalable cloud infrastructure capable of handling large volumes of concurrent visits across multiple facilities.

Benefits of telemedicine app development
When designed correctly, a telemedicine app creates value for multiple stakeholders: patients, healthcare providers, as well as clinics and healthcare organizations. Let's take a closer look at them.
For healthcare startup founders and digital health companies
A well-architected telehealth product creates a defensible market position. A focused MVP validates product-market fit before full-scale investment — and demonstrates clinical outcomes to investors and payers.
For hospital systems and clinic operators
Removes geographic barriers, reduces no-shows, and enables hybrid care models that reduce clinic overcrowding. EHR integration eliminates double documentation. Organized telehealth workflows simplify reimbursement.
For clinicians and healthcare providers
Asynchronous consultations, pre-visit messaging, and streamlined intake free up appointment time. Remote monitoring provides ongoing patient data to support proactive care decisions.
"Hybrid care models don't disrupt the workflow — they make it more effective, organized, and accessible."

Core and advanced features of a telemedicine app
A successful product starts with the right feature set — balanced between speed-to-market and long-term scalability. Most teams begin with a structured MVP and expand gradually.
Core MVP features
A well-scoped MVP focuses on a small set of features that support secure, reliable care delivery:
- Secure video consultation with end-to-end encryption and adaptive streaming
- Secure messaging for post-visit follow-ups
- Asynchronous communication to reduce unnecessary appointments
- Appointment scheduling with automated reminders
- User authentication and role-based access control
- Multi-factor authentication for all provider accounts
- Secure backend database with encryption in transit and at rest
- Basic patient and provider profiles
"An effective MVP starts small — secure communication, clear workflows, dependable data handling. Trust and compliance first, advanced capabilities later."
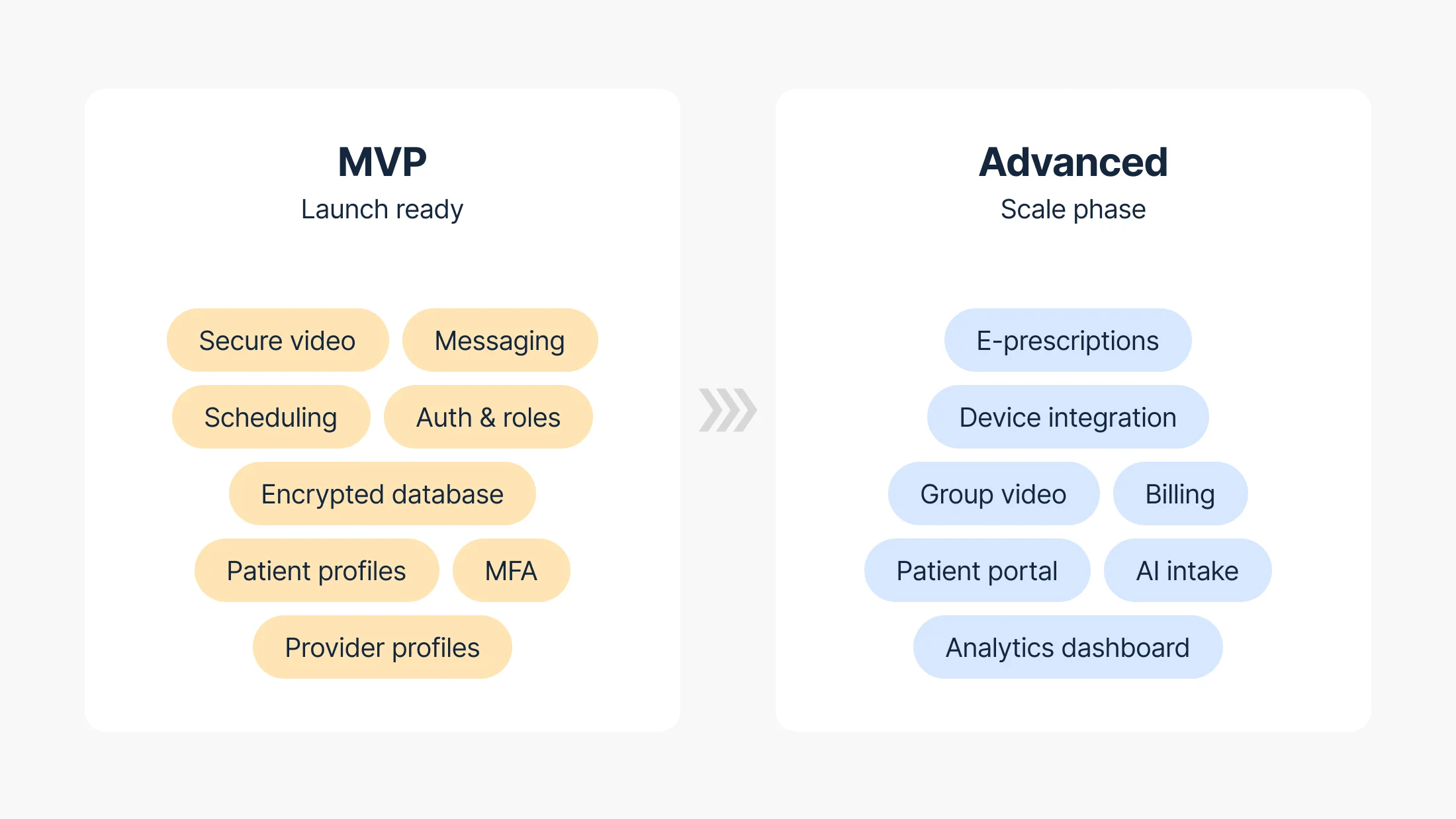
Advanced features
After validating the core experience, the next layer of development focuses on extending clinical capabilities and improving operational efficiency:
- E-prescriptions — send medication orders directly to pharmacies
- Connected device integration — wearable data flows into provider dashboards
- Group video calls — multi-party multidisciplinary consultations
- Mobile payments and subscription billing — with PCI DSS compliance
- Patient portals — visit summaries, prescriptions, test results
- Analytics dashboards — patient engagement, revenue, operational efficiency
AI & automation in telemedicine
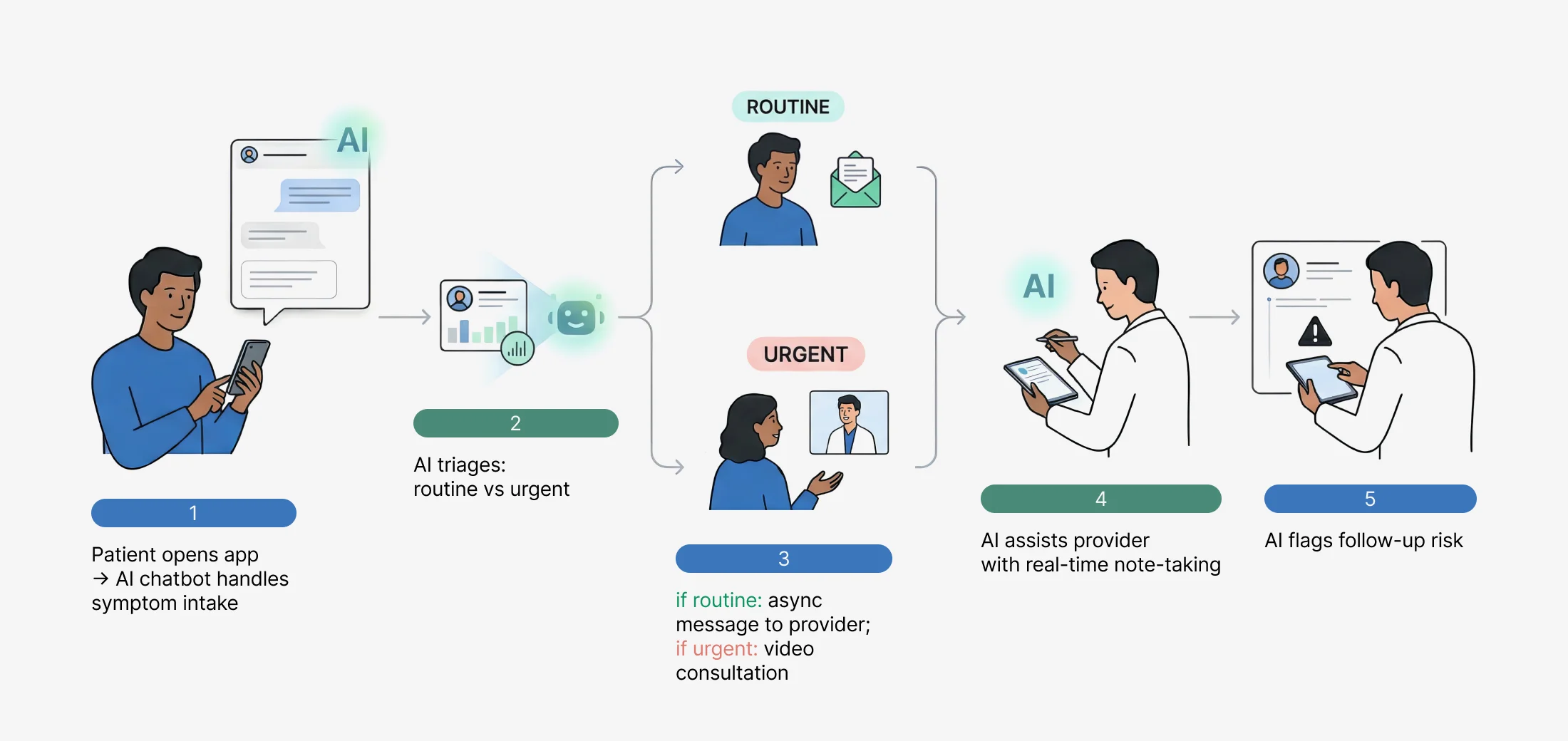
AI-powered chatbots assist with symptom intake and triage, reducing provider workload before a live consultation. Large Language Models (LLMs) can help generate structured clinical notes from consultation conversations or summarize patient histories. Scheduling systems use ML to predict cancellation risks. Predictive analytics support preventive care by identifying high-risk patients early.
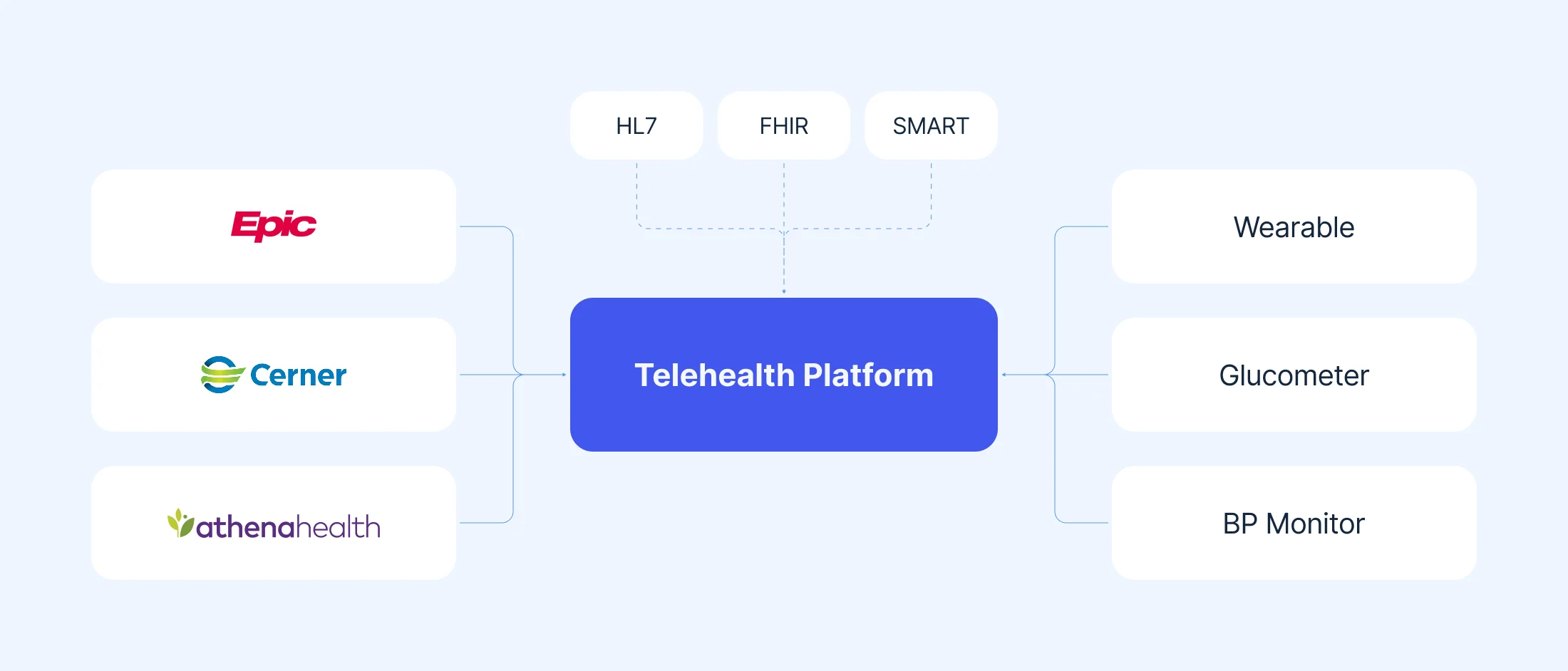
EHR/EMR integration and interoperability
Integration with existing healthcare systems is often one of the most technically complex aspects of telemedicine app development. Without interoperability, providers face double documentation and fragmented workflows.
HL7, FHIR, and SMART on FHIR
HL7 provides the structure for how data moves between platforms. FHIR builds on this, making data sharing simpler across modern applications. SMART on FHIR allows secure third-party apps to connect directly inside EHR systems without breaking existing workflows.
Common integration challenges
Legacy EHR platforms often don't support modern APIs. Data mapping inconsistencies can lead to mismatched records. Retry logic and queue systems manage temporary data exchange failures. Plan integration around specific workflows first — not every system at once.
Telemedicine app security and compliance
Building healthcare technology goes beyond innovation — it requires responsibility. Every feature, integration, and user interaction must operate within a strict regulatory and security framework. A single compliance gap creates serious legal and operational risk.
The following regulations define how telemedicine platforms must be designed, deployed, and operated:
- HIPAA (USA): Governs storage, transmission, and use of protected health information. Every architectural decision must be evaluated against HIPAA's technical safeguards.
- GDPR (EU): Sets strict rules for handling personal data across the EU — relevant for any platform serving EU patients or providers, regardless of company location.
- 21st Century Cures Act: Prohibits information blocking, mandates FHIR-based data exchange for covered entities.
- FDA oversight: Certain clinical decision-support tools require FDA review. Identifying this early prevents significant launch delays.
- PCI DSS: Applies when processing payment information within the platform.
Security best practices
In addition to regulatory requirements, security must be enforced through concrete technical and operational controls. These practices form the foundation of a secure and compliant telemedicine platform:
- End-to-end encryption for all data in transit and at rest
- TLS protocols for all data transfer between systems
- Role-based access control limiting access to essential functions only
- Multi-factor authentication for all provider accounts
- Audit logs recording who accessed data, when, and from where
- Regular penetration testing and security audits
- Incident response plans for managing breaches responsibly
- Business Associate Agreements (BAAs) with all cloud and third-party providers
"Security planning should begin during architecture design, not after development is complete."

Licensing and legal considerations in telemedicine
Legal compliance extends beyond data protection. In most jurisdictions, providers must be licensed in the state or country where the patient is located at the time of consultation.
Telemedicine platforms must also account for jurisdiction-specific legal requirements that directly affect product design and operations:
- Prescribing regulations vary by region, especially for controlled substances
- Telehealth consent requirements differ across states and countries
- Cross-border care adds regulatory complexity that must be addressed in product architecture
- Recording consultations may require explicit patient consent, depending on the jurisdiction
In practice, these considerations are best addressed during product planning, not after development has started.
Telemedicine app design example: myReha
Neurological rehabilitation doesn't end at hospital discharge. Patients recovering from stroke, Alzheimer's, or multiple sclerosis need months of ongoing therapy — often at home, without supervision, and at an older age. myReha, a Vienna-based digital therapeutics company (now part of nyra health), developed a tablet app offering adaptive, game-like exercises. Although the clinical model was effective, the product experience struggled to keep pace as the solution expanded.
Therapists needed quicker access to patient data, while patients required an interface that supported both their condition and their dignity. Simultaneously, the product was shifting from tablets to smartphones and from hospital settings to home care. Halo Lab worked on this challenge for 17 months, redesigning the therapist dashboard (nyra.insights) around one core principle: clinicians should assess patient status in seconds, not clicks.
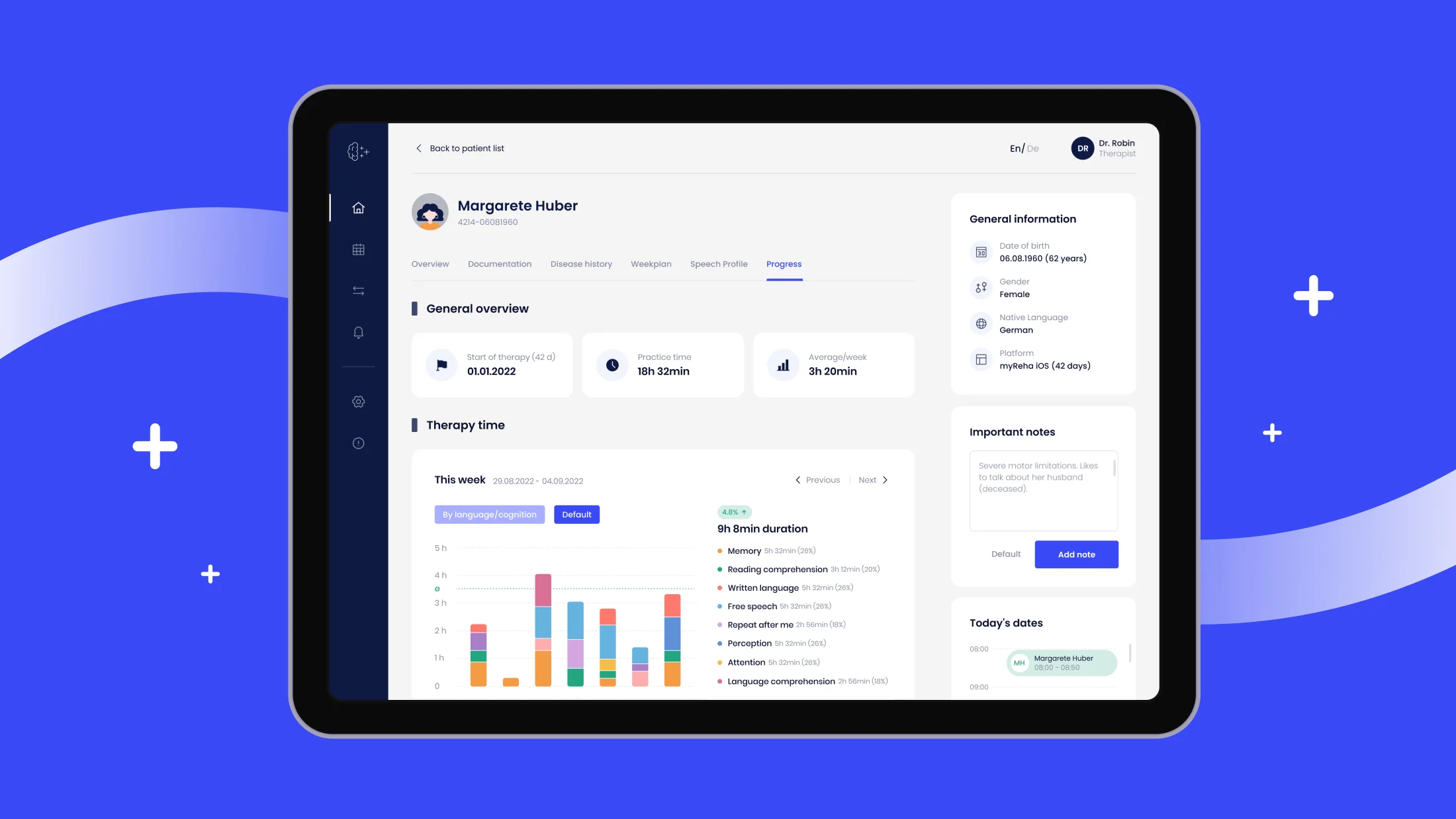
On the patient side, every decision prioritized accessibility — high-contrast visuals for stroke-related impairments, a single-day therapy view to reduce cognitive load, and neutral illustrations instead of patronizing visuals. As the app transitioned to smartphones, layouts were adapted selectively to maintain exercise quality. The result is a cohesive design system spanning multiple devices and a growing network of rehabilitation clinics across Europe.
Telemedicine app development process
Building a healthcare product requires structured phases. Here is how our team at Halo Lab approaches each stage — and why the sequence matters as much as the work itself.
Phase 1: Discovery and product strategy
This phase sets the direction for the entire project. We explore target users, map clinical workflows, and establish the regulatory scope before making any design decisions.
Projects that skip or rush discovery often require expensive rebuilds within the first few months. In practice, many teams bring in external expertise at this stage to align product decisions with regulatory and operational constraints before development begins — often through structured healthcare IT consulting.
Phase 2: MVP scoping
During this phase, we define what belongs in the first release, what can follow, and what is being introduced too early. Scope creep at the MVP stage is one of the most common reasons healthcare products miss their launch window.
A clearly defined MVP development scope helps teams prioritize effectively and build a phased roadmap that supports both validation and future growth.
Phase 3: UI/UX design for healthcare
Healthcare UX has constraints that standard product design doesn't. Users include elderly patients, time-pressured clinicians, and administrators managing multiple providers. Accessibility features — larger text, screen reader compatibility, clear navigation — are not optional in healthcare. When AI features are part of the product, clinical trust must be designed in from the start — covering explainability, confidence signals, and override architecture. Our healthcare UI/UX design services ensure interfaces meet both usability and regulatory standards.
Phase 4: Development and API integration
At this phase, our team brings together three coordinated layers: backend infrastructure for secure data processing, frontend interfaces for patients and providers, and third-party integrations for video, messaging, payments, and EHRs. Compliance controls should be built into the architecture from the start — a principle that underpins effective healthcare software development.
Phase 5: Testing, compliance validation, and QA
This stage includes functional checks, usability assessments, security reviews, compliance validation, and stress testing under peak load. We validate each layer before launch to ensure the system performs reliably in real clinical environments. This level of validation is central to healthcare software testing.
Phase 6: Deployment, launch, and ongoing maintenance
The final stage includes mobile app publication, secure cloud infrastructure configuration, and launch monitoring. After release, our teams typically support the platform through ongoing security audits, compliance updates, and feature development informed by real user behavior and operational feedback.

Tech stack and architecture for telemedicine app development
Infrastructure decisions at the architecture stage directly affect performance, compliance, and long-term costs. A typical telemedicine architecture includes the following components:
- Cloud: AWS or Google Cloud with HIPAA-eligible services and BAAs.
- Backend: Node.js, Python, or Java for secure APIs and data exchange.
- Frontend: React Native for cross-platform mobile; React or Angular for provider dashboards.
- Video: Twilio or Agora for real-time communication and adaptive streaming.
- Database: PostgreSQL or MongoDB with encryption at rest.
- Reliability: Load balancers, autoscaling, and real-time monitoring tools.

Team structure: who you need to build a telemedicine app
A telemedicine platform depends on coordinated expertise across product, engineering, and healthcare domains. The following roles typically form the core team:
- Product manager — scope, priorities, roadmap milestones.
- Healthcare domain specialists — ensure workflows reflect real clinical standards, not assumptions.
- Backend developers — APIs, authentication, database logic.
- Frontend developers — patient and provider-facing interfaces.
- DevOps engineers — cloud infrastructure, CI/CD, security controls.
- QA specialists — functionality, performance, and security testing.
- Compliance consultants — regulatory review and gap identification.
- UI/UX designers — accessibility and usability across patient groups.
- Integration specialists — EHR connectivity and interoperability (mid-market and enterprise).
"When all roles work together in a coordinated structure, teams reduce delays and prevent the compliance gaps that cause cost overruns."

How much does it cost to build a telehealth app?
The full picture of app development cost varies significantly based on feature depth, integration requirements, and compliance scope.
Beyond initial development: budget for monthly cloud hosting, monitoring, security updates, and compliance maintenance as the platform scales.
{{banner}}

Common challenges — and how to avoid them
Healthcare software presents specific technical and operational challenges, and identifying them early helps ensure a smoother, more successful telemedicine app development.
Starting compliance late
Teams that treat HIPAA and GDPR as a final checklist routinely discover they need to rebuild core data infrastructure. Start compliance planning before the first design decision.
Underestimating EHR integration complexity
Legacy EHR systems don't behave like modern APIs. Plan integration around specific workflows first — not all systems at once — and budget time for repeated testing and data mapping.
Over-scoping the MVP
Too many features in the first release is the most common reason healthcare MVPs miss their launch window. Define the minimum to validate clinical demand, then expand.
Ignoring video performance at scale
Adaptive streaming and fallback mechanisms are baseline requirements. Stress test before launch — not after the first failure under real-world load.
Weak patient onboarding
Opaque privacy policies and confusing consent flows erode confidence before the first consultation. Simple onboarding is especially critical for elderly patients and users with limited technical comfort.
"Early attention to privacy, compliance, and integration scope lays the foundation for secure, reliable, and trusted telehealth growth."

The future of telemedicine app development
Telehealth continues to evolve. What does the future hold for those entering this field? Here are some trends you can expect.
AI-driven virtual care
AI agents are expected to support triage, intake, and documentation at scale, reducing administrative burden on providers. Predictive models will identify high-risk patients earlier. Teams building for this now will have a significant advantage over those who retrofit AI later. Our AI integration services can help implement these tools responsibly and in line with regulatory expectations.
Mental health and chronic care growth
Behavioral health will continue performing exceptionally well, driven by strong remote therapy and psychiatric demand. Chronic disease management through remote monitoring is expanding as providers seek cost-effective ways to support long-term conditions outside traditional clinics.
Interoperability as a competitive advantage
Stronger FHIR-based data exchange and anti-information-blocking regulations are making interoperability a market expectation, not just a technical nicety. Platforms that connect seamlessly with the broader healthcare data ecosystem will win in enterprise and health system sales.
Inclusive healthcare UX
WCAG accessibility standards, voice recognition, and screen reader compatibility will become baseline expectations. Platforms easy for everyone to use — not just the tech-comfortable — will retain patients better.
Predictive analytics and preventive care
Preventive care models gain traction as health data becomes more accessible. Predictive analytics helps providers identify potential risks before conditions escalate — reducing hospital readmissions and supporting better long-term outcomes.

Build a system, not just features
Healthcare systems face increasing demand and limited clinical capacity. Telemedicine apps offer a structured way to extend access to care, but only when built with the right architecture, compliance posture, and clinical workflows from day one. The teams that succeed in telemedicine app development are the ones that plan it as a system, not a feature collection.

Writing team:
Have a project
in your mind?
Let’s communicate.
in your mind?
Let’s communicate.

Frequently Asked Questions
What features are essential for a telemedicine MVP?
Secure video conferencing, encrypted messaging, appointment scheduling, user authentication with role-based access, and a secure backend database. Everything else follows once clinical demand is validated.
How long does it take to build a telemedicine app?
A focused MVP may take 10–14 weeks. Platforms with EHR integrations or enterprise requirements usually take 6–9 months or longer. Timelines depend heavily on integration complexity and how clearly the scope is defined before development starts.
What affects telemedicine app development cost the most?
Integration complexity. Connecting to EHRs, ensuring compliance at every layer, adding AI or monitoring features, and planning for scalability all require significantly more time. MVP scope clarity before development starts also has a major impact on the final cost.
Do telemedicine apps require regulatory approval?
Apps providing clinical decision support or connecting with regulated devices must comply with HIPAA and applicable regional laws. Some tools require FDA review if they influence clinical decisions. Identifying this early prevents costly launch delays.
Can a telemedicine app scale to an enterprise level?
Yes — with the right architecture from the start. Multi-role dashboards, advanced permissions, audit trails, enterprise SSO, and high-concurrency infrastructure need to be planned in from day one, not retrofitted.




















.webp)
.png)






